South Africa’s planned health policy overhaul through a multi-billion dollar national insurance scheme has drawn mixed responses as the state attempts to tackle its ailing public hospitals.
The bold proposal, published on Friday for public comment, aims to close the gap with expensive private care and provide universal health coverage at a cost of 255 billion rand (US$17 billion) by 2025.
The 14-year National Health Insurance (NHI) vision is to improve shoddy public facilities used by 84 percent of South Africans, rope in accredited private providers and draw wealthier patients who are on medical schemes.
“We were worried initially ... we didn’t know what was coming,” said Norman Mabasa, chairman of doctors body the South African Medical Association.
“We would have been concerned if we were told how it would be modeled, but we are happy if we are going to participate on how it is going to be modeled,” he said.
South Africa inherited 14 health systems from the apartheid era, and the merged system has limped along post-1994 to spark a parallel industry of private, but pricey quality care, which the state says is unfair and unsustainable.
The country’s health spend accounts for 8.5 percent of GDP with state spending nearly matched by that of medical insurance schemes who cover just 17.6 percent of about 50 million people, with only one in 10 blacks as members.
Health economist Alex van den Heever of Wits University said South Africa had “appalling” health outcomes despite the amount it was spending and that the proposal lacked a specific blueprint for reform.
“What I can find is that there is a defensiveness about why we have a failing health system and then kind of a claim that we will, through extra money, turn this around,” Van den Heever said. “The problem with the public system goes way beyond money.”
The government admits that beefing up services is key to the NHI’s success, but Van den Heever was critical.
“I have seen nothing in those proposals that really address the fundamental core concerns that have become very evident in the public system,” he said. “It’s [the public system] largely designed to fail in that it essentially lacks a coherent governance and accountability framework and its actual institutional model is weak.”
The plan is costed at 125 billion rand for next year, rising to 214 billion in 2020, but the 59-page paper does not say how this will be bankrolled.
A possible mix of funding includes the fiscus, employers and individuals — with a mandatory contribution cited — but the exact details will only be known in the next six months ahead of a pilot phase in 10 areas next April.
The number of people likely to retain private schemes has not yet been quantified, said Cobus Venter, director of consultancy Econex.
“Therefore the assumption that only 6.2 percent of GDP will be spent on health is false as this only reflects the increased level of expenditure in the public sector, even incorporating some private providers,” he said.

‘IN A DIFFERENT PLACE’: The envoy first visited Shanghai, where he attended a Chinese basketball playoff match, and is to meet top officials in Beijing tomorrow US Secretary of State Antony Blinken yesterday arrived in China on his second visit in a year as the US ramps up pressure on its rival over its support for Russia while also seeking to manage tensions with Beijing. The US diplomat tomorrow is to meet China’s top brass in Beijing, where he is also expected to plead for restraint as Taiwan inaugurates president-elect William Lai (賴清德), and to raise US concerns on Chinese trade practices. However, Blinken is also seeking to stabilize ties, with tensions between the world’s two largest economies easing since his previous visit in June last year. At the
Nearly half of China’s major cities are suffering “moderate to severe” levels of subsidence, putting millions of people at risk of flooding, especially as sea levels rise, according to a study of nationwide satellite data released yesterday. The authors of the paper, published by the journal Science, found that 45 percent of China’s urban land was sinking faster than 3mm per year, with 16 percent at more than 10mm per year, driven not only by declining water tables, but also the sheer weight of the built environment. With China’s urban population already in excess of 900 million people, “even a small portion
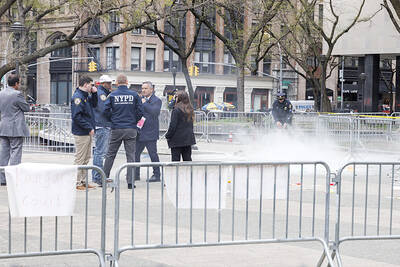
UNSETTLING IMAGES: The scene took place in front of TV crews covering the Trump trial, with a CNN anchor calling it an ‘emotional and unbelievably disturbing moment’ A man who doused himself in an accelerant and set himself on fire outside the courthouse where former US president Donald Trump is on trial has died, police said yesterday. The New York City Police Department (NYPD) said the man was declared dead by staff at an area hospital. The man was in Collect Pond Park at about 1:30pm on Friday when he took out pamphlets espousing conspiracy theories, tossed them around, then doused himself in an accelerant and set himself on fire, officials and witnesses said. A large number of police officers were nearby when it happened. Some officers and bystanders rushed

Beijing is continuing to commit genocide and crimes against humanity against Uyghurs and other Muslim minorities in its western Xinjiang province, U.S. Secretary of State Antony Blinken said in a report published on Monday, ahead of his planned visit to China this week. The State Department’s annual human rights report, which documents abuses recorded all over the world during the previous calendar year, repeated language from previous years on the treatment of Muslims in Xinjiang, but the publication raises the issue ahead of delicate talks, including on the war in Ukraine and global trade, between the top U.S. diplomat and Chinese