Although the number of health workers has doubled in the past two decades, the nation still faces a shortage of staff in the fields of internal medicine, surgery, gynecology, pediatrics and emergency care, academics and health professionals said at a seminar last week.
Chiang Tung-liang (江東亮), a professor at National Taiwan University’s (NTU) College of Public Health, said that the reasons behind the staff shortage in the five fields were “very complicated” and could only be resolved by understanding the root of the problem.
According to his data analysis, covering the period from 1990 to 2010, the number of health workers in pediatrics has increased by 50 to 60 percent, with the number of doctors setting up their own clinics rising by 20 percent, Chiang said.
The increasing availability of pediatric clinics in small towns with low population densities has seen these clinics branching out from their own field of specialty, Chiang said.
A declining birthrate — down 20 percent over the past decade — corresponded with a 10 percent increase in the number of adult patients, reinforcing the trend, Chiang said.
Taiwan Pediatric Association director-general Lee Ping-ing (李秉穎) said that pediatricians are generally viewed by hospitals as a bad investment, because the overhead for maintaining pediatricians is high, but the income they generate is relatively low.
Lee said the problem lay with the Bureau of National Health Insurance, which he said had listened to other agencies, but failed to respect the opinions of medical professionals.
Lee cited as an example the difference between having a child and an adult undergo a nuclear magnetic resonance (NMR) procedure.
The adult will quietly stay put, but the child will not, he said.
Anesthesia may have to be administered for the procedure to be successful, but the bureau has removed such funding, he said.
The bureau has not factored in special circumstances that caring for children may entail, which means patients have to pay out of their own pockets, he added.
Comparing the payout for pediatric health checkups in different countries, Lee said that both Hong Kong and Japan had payout amounts three times higher than Taiwan’s, while South Korea’s was 2.5 times that of Taiwan.
Pediatricians also have to shoulder the responsibility of administering public-funded vaccines, but they have to fight tooth-and-nail for the bureau to reimburse checkup fees in their own clinics, Lee said.
This is just another example of “the higher the quality of medical care provided, the lower the income [of the provider],” he said.
Chiang suggested that the bureau should promote the concept of calculating expenses based on the individual receiving care, or the quality of treatment being provided.
The government should also encourage the forming of medical teams composed of pediatricians, obstetricians, internal medicine practitioners and family doctors.
With such a team, medical care would be provided for mothers and children from birth through their teenage years, Chiang said.
The association and 46 other organizations last year called on the presidential candidates to pass such a system, also known as the “children’s care doctor” system, Chiang said.
However, there has been no progress on the issue to date.
Both Tien and Huang voiced their support for the system, saying it would not only help provide healthcare guarantees for children, it would also be a great boon to new mothers, adding that they are considering a trial implementation of the system.
Aside from health professionals and academics, the seminar on Nov. 18 was attended by Department of Health Minister Chiu Wen-ta (邱文達), Bureau of National Health Insurance Director-General Huang San-kuei (黃三桂) and lawmakers across party lines.

A group of Taiwanese-American and Tibetan-American students at Harvard University on Saturday disrupted Chinese Ambassador to the US Xie Feng’s (謝鋒) speech at the school, accusing him of being responsible for numerous human rights violations. Four students — two Taiwanese Americans and two from Tibet — held up banners inside a conference hall where Xie was delivering a speech at the opening ceremony of the Harvard Kennedy School China Conference 2024. In a video clip provided by the Coalition of Students Resisting the CCP (Chinese Communist Party), Taiwanese-American Cosette Wu (吳亭樺) and Tibetan-American Tsering Yangchen are seen holding banners that together read:

UNAWARE: Many people sit for long hours every day and eat unhealthy foods, putting them at greater risk of developing one of the ‘three highs,’ an expert said More than 30 percent of adults aged 40 or older who underwent a government-funded health exam were unaware they had at least one of the “three highs” — high blood pressure, high blood lipids or high blood sugar, the Health Promotion Administration (HPA) said yesterday. Among adults aged 40 or older who said they did not have any of the “three highs” before taking the health exam, more than 30 percent were found to have at least one of them, Adult Preventive Health Examination Service data from 2022 showed. People with long-term medical conditions such as hypertension or diabetes usually do not

POLICE INVESTIGATING: A man said he quit his job as a nurse at Taipei Tzu Chi Hospital as he had been ‘disgusted’ by the behavior of his colleagues A man yesterday morning wrote online that he had witnessed nurses taking photographs and touching anesthetized patients inappropriately in Taipei Tzu Chi Hospital’s operating theaters. The man surnamed Huang (黃) wrote on the Professional Technology Temple bulletin board that during his six-month stint as a nurse at the hospital, he had seen nurses taking pictures of patients, including of their private parts, after they were anesthetized. Some nurses had also touched patients inappropriately and children were among those photographed, he said. Huang said this “disgusted” him “so much” that “he felt the need to reveal these unethical acts in the operating theater
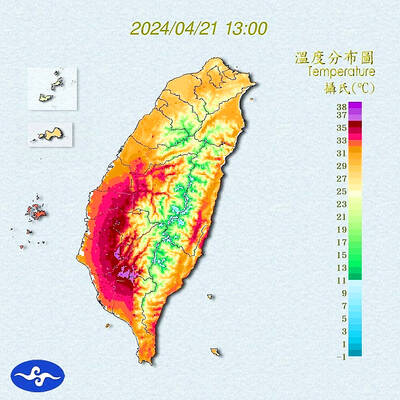
Heat advisories were in effect for nine administrative regions yesterday afternoon as warm southwesterly winds pushed temperatures above 38°C in parts of southern Taiwan, the Central Weather Administration (CWA) said. As of 3:30pm yesterday, Tainan’s Yujing District (玉井) had recorded the day’s highest temperature of 39.7°C, though the measurement will not be included in Taiwan’s official heat records since Yujing is an automatic rather than manually operated weather station, the CWA said. Highs recorded in other areas were 38.7°C in Kaohsiung’s Neimen District (內門), 38.2°C in Chiayi City and 38.1°C in Pingtung’s Sandimen Township (三地門), CWA data showed. The spell of scorching