The Bureau of National Health Insurance yesterday announced that Diagnosis Related Groups (DRGs) will be formed from Sept. 1, but doctors expressed concern that they could lead to patients receiving inadequate care.
DRGs are a new policy that determines how National Health Insurance covers a patient’s expenses while in hospital.
DRGs provide a way of relating the type of patients treated by a hospital to the costs incurred by the hospital. Groups of patients have similar demographic, diagnostic and therapeutic attributes that determine the resources they need.
The process of fully implementing DRGs is expected to take six years. When the new policy is launched on Sept. 1, a total of 111 categories will be established.
The bureau said that another 856 categories would be completed by the end of the six-year period.
“DRGs will help us avoid unnecessary waste of medical resources,” said Tsai Shu-ling (蔡淑鈴), manager of the bureau’s Medical Affairs Section.
“With the new policy, hospitals will be able to avoid unnecessary waste and offer more efficient help and medical treatment,” Tsai said.
She said that under the current system, many patients spend time in hospital waiting for check-ups or surgery. The National Health Insurance has to cover all the expenses for hospital stays, even though patients are often waiting to see a doctor or receive treatment.
“If we pay the same amount to a hospital no matter whether the patient stays for one day or one week, the hospital, of course, will speed up their work and treat the patient as soon as possible. This is the idea behind the new policy,” Tsai said.
Doctors, however, expressed concern over the new policy.
“Say a patient develops pneumonia, high blood pressure and diabetes at the same time. Under the new policy, it is possible that the bureau will not pay the necessary expenses for high blood pressure and diabetes if the patient only fits one category, according to the prescription by the doctor,” said Wu Der-lang (吳德朗), chairman of the Taiwan Hospital Association.
Wu said hospitals may refuse to treat patients with multiple illnesses, or will ask the patient to undergo treatment for one illness, check out of hospital, and then re-register for the second illness.
“If the hospital does not do this, it will not be able to receive extra reimbursement from the bureau,” Wu said.

A group of Taiwanese-American and Tibetan-American students at Harvard University on Saturday disrupted Chinese Ambassador to the US Xie Feng’s (謝鋒) speech at the school, accusing him of being responsible for numerous human rights violations. Four students — two Taiwanese Americans and two from Tibet — held up banners inside a conference hall where Xie was delivering a speech at the opening ceremony of the Harvard Kennedy School China Conference 2024. In a video clip provided by the Coalition of Students Resisting the CCP (Chinese Communist Party), Taiwanese-American Cosette Wu (吳亭樺) and Tibetan-American Tsering Yangchen are seen holding banners that together read:

UNAWARE: Many people sit for long hours every day and eat unhealthy foods, putting them at greater risk of developing one of the ‘three highs,’ an expert said More than 30 percent of adults aged 40 or older who underwent a government-funded health exam were unaware they had at least one of the “three highs” — high blood pressure, high blood lipids or high blood sugar, the Health Promotion Administration (HPA) said yesterday. Among adults aged 40 or older who said they did not have any of the “three highs” before taking the health exam, more than 30 percent were found to have at least one of them, Adult Preventive Health Examination Service data from 2022 showed. People with long-term medical conditions such as hypertension or diabetes usually do not

POLICE INVESTIGATING: A man said he quit his job as a nurse at Taipei Tzu Chi Hospital as he had been ‘disgusted’ by the behavior of his colleagues A man yesterday morning wrote online that he had witnessed nurses taking photographs and touching anesthetized patients inappropriately in Taipei Tzu Chi Hospital’s operating theaters. The man surnamed Huang (黃) wrote on the Professional Technology Temple bulletin board that during his six-month stint as a nurse at the hospital, he had seen nurses taking pictures of patients, including of their private parts, after they were anesthetized. Some nurses had also touched patients inappropriately and children were among those photographed, he said. Huang said this “disgusted” him “so much” that “he felt the need to reveal these unethical acts in the operating theater
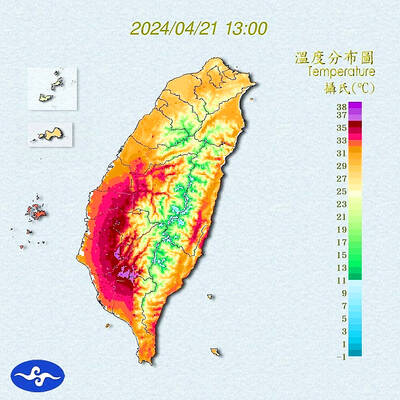
Heat advisories were in effect for nine administrative regions yesterday afternoon as warm southwesterly winds pushed temperatures above 38°C in parts of southern Taiwan, the Central Weather Administration (CWA) said. As of 3:30pm yesterday, Tainan’s Yujing District (玉井) had recorded the day’s highest temperature of 39.7°C, though the measurement will not be included in Taiwan’s official heat records since Yujing is an automatic rather than manually operated weather station, the CWA said. Highs recorded in other areas were 38.7°C in Kaohsiung’s Neimen District (內門), 38.2°C in Chiayi City and 38.1°C in Pingtung’s Sandimen Township (三地門), CWA data showed. The spell of scorching