When Thida Win contracted HIV after selling her body on the Yangon streets, it was her fellow sex workers that she turned to, not Myanmar’s crumbling health service.
The Top project, run almost entirely by those in the sex trade, gave her treatment, a place to be herself away from the dual stigma of HIV and prostitution — and eventually a job.
“I am now a health worker for my community and I can forget I am positive. I am so proud to work for the programs, I will work for them for my whole life,” the 33-year-old said.
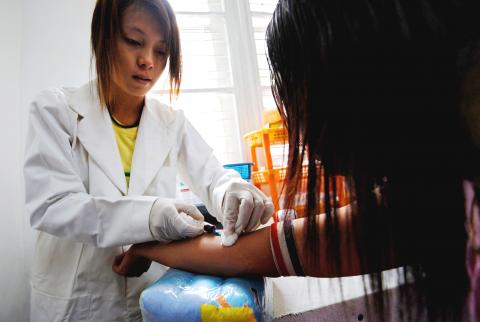
Photo: AFP
Top and similar projects are a vital resource in army-dominated Myanmar, where a chronically underfunded health service, large itinerant populations and poor education fuel one of Asia’s worst HIV epidemics.
“When I was diagnosed I was pregnant and they told me how to find a safe way for the baby. So the child is negative and I am so happy,” Thida Win said.
Nearly one in five of Myanmar’s estimated 60,000 sex workers were infected with HIV in 2008.
A UN report from August last year said legal constraints and discrimination made it hard to reach those in the trade, which is illegal. Surveys suggested police even used condoms as evidence for arrest.
Top founder and director Habib Rahman said providing a place free from taboos and letting people share their problems with contemporaries was a key aim for the project.
“Even the cleaner comes from the sex worker community, the counselors are also sex workers. That’s one of the reasons I decided to recruit from the community — because there should not be any stigma and discrimination,” he said.
Rahman said many women enter sex work without knowing about the risks.
“In general in Myanmar I do not think there is any sex education in school,” he said.
The project recruits former and current sex workers to help educate others about HIV, spreading the message from a position of trust within the community.
“We cannot tell anyone to stop selling sex even though they are positive, but what we do is tell them how they can keep healthy and protect the client by using condoms,” Rahman said.
He said Top’s part-time “peer educators,” who chose to continue in the sex trade, were encouraged to always use protection, while full-time employees were instructed to stop selling sex altogether.
HIV transmission in Myanmar occurs “primarily through high-risk sexual contact between sex -workers and their clients,” as well as men who have sex with men and their partners, according to the UN report.
It said while injecting drug users have the highest HIV prevalence, at 36 percent, they are also likely to pay for sex and “this interaction may refuel the sex-work-driven epidemic.”
Years of neglect by the ruling generals — Myanmar spent just 0.9 percent of its budget on health in 2007 — have left foreign donors facilitating most of the country’s HIV treatment.
A new government, which came into power after controversial elections in November last year, has raised hopes of more investment from overseas donors — but not the state, which is expected to spend around 20 percent of outlay on the army this year.
In 2009, the UN estimated 240,000 people in Myanmar were living with the virus and while there have been improvements, the situation remains worrying with prevalence rates the third-highest in Asia after Thailand and Papua New Guinea.
“The HIV epidemic in Myanmar is on a decreasing trend and among the key population groups it is also reducing — but it is still really quite high,” said Soe Naing of UNAIDS in Myanmar.
He said some state provision for HIV treatment does exist in big cities, “but of course the standards and situations are not ideal. People are reluctant to go to them because of privacy issues and quality.”
Top clinics provide everything from testing and counseling to routine medical care.
Last year, it gave treatment and consultation to 11,770 female sex workers and 10,727 men. It also accounted for 40 percent and 82 percent of all HIV tests for those groups respectively in the country.
The program, which was formed by Population Services International seven years ago, now employs 350 people — 95 percent of whom are from the sex worker community and men who have sex with men — in 19 towns and cities.
In Myanmar, where the US estimates around a third of people were below the poverty line in 2007, money worries are likely to continue to drive people into sex work.
Thida Win, who was still a university student when she first sold sex, said the financial burden of marriage and children only pushed her further into the trade.
“I got my degree with sex work, I supported my family very well with sex work,” said the chemistry graduate, who said her earnings still help support seven family members.

Eleven people, including a former minister, were arrested in Serbia on Friday over a train station disaster in which 16 people died. The concrete canopy of the newly renovated station in the northern city of Novi Sad collapsed on Nov. 1, 2024 in a disaster widely blamed on corruption and poor oversight. It sparked a wave of student-led protests and led to the resignation of then-Serbian prime minister Milos Vucevic and the fall of his government. The public prosecutor’s office in Novi Sad opened an investigation into the accident and deaths. In February, the public prosecutor’s office for organized crime opened another probe into

RISING RACISM: A Japanese group called on China to assure safety in the country, while the Chinese embassy in Tokyo urged action against a ‘surge in xenophobia’ A Japanese woman living in China was attacked and injured by a man in a subway station in Suzhou, China, Japanese media said, hours after two Chinese men were seriously injured in violence in Tokyo. The attacks on Thursday raised concern about xenophobic sentiment in China and Japan that have been blamed for assaults in both countries. It was the third attack involving Japanese living in China since last year. In the two previous cases in China, Chinese authorities have insisted they were isolated incidents. Japanese broadcaster NHK did not identify the woman injured in Suzhou by name, but, citing the Japanese

YELLOW SHIRTS: Many protesters were associated with pro-royalist groups that had previously supported the ouster of Paetongtarn’s father, Thaksin, in 2006 Protesters rallied on Saturday in the Thai capital to demand the resignation of court-suspended Thai Prime Minister Paetongtarn Shinawatra and in support of the armed forces following a violent border dispute with Cambodia that killed more than three dozen people and displaced more than 260,000. Gathered at Bangkok’s Victory Monument despite soaring temperatures, many sang patriotic songs and listened to speeches denouncing Paetongtarn and her father, former Thai prime minister Thaksin Shinawatra, and voiced their backing of the country’s army, which has always retained substantial power in the Southeast Asian country. Police said there were about 2,000 protesters by mid-afternoon, although

MOGAMI-CLASS FRIGATES: The deal is a ‘big step toward elevating national security cooperation with Australia, which is our special strategic partner,’ a Japanese official said Australia is to upgrade its navy with 11 Mogami-class frigates built by Japan’s Mitsubishi Heavy Industries, Australian Minister for Defence Richard Marles said yesterday. Billed as Japan’s biggest defense export deal since World War II, Australia is to pay US$6 billion over the next 10 years to acquire the fleet of stealth frigates. Australia is in the midst of a major military restructure, bolstering its navy with long-range firepower in an effort to deter China. It is striving to expand its fleet of major warships from 11 to 26 over the next decade. “This is clearly the biggest defense-industry agreement that has ever