Symptomatological and neuropsychological hints can be used to predict psychosis, attending psychiatrist at National Taiwan University Hospital Liu Chen-chung (劉震鐘) said yesterday.
Liu made the remarks at this year’s International Symposium on Brain and Mind Sciences in Taipei, which focused on early detection and treatment of schizophrenia.
In his presentation on the neuropsychological study of early schizophrenia, Liu made public the results of a follow-up study on the psychopathological progress of early schizophrenia-like disorders, a five-year project sponsored by the National Health Research Institute from 2006 to 2010.
Led by National Taiwan University professor emeritus of psychiatry Hwu Hai-gwo (胡海國), the project aimed to follow not only participants with first-episode psychosis (FEP) or ultra-high-risk (UHR) for psychosis, now also called attenuated psychosis syndrome (APS), but also those at intermediate risk and marginal risk of psychosis.
“It echoes a recent proposal that if you want to monitor the pathogenesis of schizophrenia, [you should] not only focus on the late prodromal state like APS,” but also the earlier stages, Liu said.
By conducting a combination of neuropsychological tests, besides the FEP group, putative pre-psychotic participants were categorized into a UHR group, intermediate risk group (IRG) and marginal risk group, with the UHR group divided into those who transitioned into full-blown psychosis during the follow-up (UHR positive) and those who did not (UHR negative).
A total of 318 participants, divided into five groups, including the four mentioned above and a control group, were given baseline assessments, Liu said.
Liu said that although it was expected that there would be a gradient in the wellbeing of neurocognitive function among the groups, the result “was not so clear.”
The FEP, UHR and IRG groups all manifested verbal memory and processing speed deficits.
“Even [the participants who had been categorized to be at] a very early stage, the MR stage … showed some cognitive declines,” Liu said.
And while the FEP group performed worse among the clinical subjects, in terms of the test results, “the difference among the other three groups was not so significant,” Liu added.
“In some indicators, the UHR negative performed even worse than the UHR positive,” Liu added. “The baseline neurocognitive function of UHR subjects [thus] provided limited evidence to differentiate those who converted to FEP from those who did not later on.”
“And this is why we need to dig into other biomarkers,” such as the underlying neural mechanism causing the emergence of psychosis, “to get stronger predictors,” Liu said.

Considering that most countries issue more than five denominations of banknotes, the central bank has decided to redesign all five denominations, the bank said as it prepares for the first major overhaul of the banknotes in more than 24 years. Central bank Governor Yang Chin-lung (楊金龍) is expected to report to the Legislative Yuan today on the bank’s operations and the redesign’s progress. The bank in a report sent to the legislature ahead of today’s meeting said it had commissioned a survey on the public’s preferences. Survey results showed that NT$100 and NT$1,000 banknotes are the most commonly used, while NT$200 and NT$2,000

The Centers for Disease Control (CDC) yesterday reported the first case of a new COVID-19 subvariant — BA.3.2 — in a 10-year-old Singaporean girl who had a fever upon arrival in Taiwan and tested positive for the disease. The girl left Taiwan on March 20 and the case did not have a direct impact on the local community, it said. The WHO added the BA.3.2 strain to its list of Variants Under Monitoring in December last year, but this was the first imported case of the COVID-19 variant in Taiwan, CDC Deputy Director-General Lin Ming-cheng (林明誠) said. The girl arrived in Taiwan on

South Korea is planning to revise its controversial electronic arrival card, a step Taiwanese officials said prompted them to hold off on planned retaliatory measures, a South Korean media report said yesterday. A Yonhap News Agency report said that the South Korean Ministry of Foreign Affairs is planning to remove the “previous departure place” and “next destination” fields from its e-arrival card system. The plan, reached after interagency consultations, is under review and aims to simplify entry procedures and align the electronic form with the paper version, a South Korean ministry official said. The fields — which appeared only on the electronic form
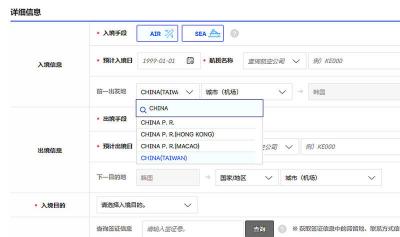
The Ministry of Foreign Affairs (MOFA) is suspending retaliation measures against South Korea that were set to take effect tomorrow, after Seoul said it is updating its e-arrival system, MOFA said today. The measures were to be a new round of retaliation after Taiwan on March 1 changed South Korea's designation on government-issued alien resident certificates held by South Korean nationals to "South Korea” from the "Republic of Korea," the country’s official name. The move came after months of protests to Seoul over its listing of Taiwan as "China (Taiwan)" in dropdown menus on its new online immigration entry system. MOFA last week