Lying in the darkened doctor's office, Kate Hoffman stared at the image of the 11-week-old fetus inside her on the ultrasound screen, a tiny ghost with a big head. It would have been so sweet, Hoffman said, if something had not been so clearly wrong.
Hoffman's first three children had been healthy and she was sure this one would be, too. She was not planning to have the amniocentesis procedure often used to test for fetal health problems, preferring to avoid even the slightest risk that the insertion of a needle into her uterus would cause her to miscarry.

PHOTO: NY TIMES
But when her doctor told her there was a new way to assess the chance of certain abnormalities with no risk of miscarriage -- a blood test and special sonogram -- she happily made an appointment.
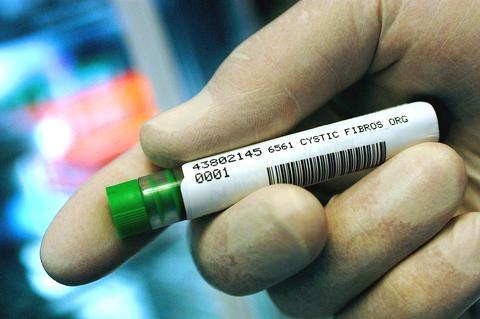
PHOTO: NY TIMES
The result, signaling that the child had a high chance of having Down syndrome, thrust Hoffman and her husband into a growing group of prospective parents who have learned far more about the health of their fetus than was possible even three years ago.
Fetal genetic tests are now routinely used to diagnose diseases as well known as cystic fibrosis and as obscure as fragile X, a form of mental retardation. High-resolution sonograms can detect life-threatening defects like brain cysts as well as treatable conditions like a small hole in the heart or a cleft palate sooner and more reliably than previous generations of the technology. And the risk of Down syndrome, one of the most common birth defects, can be reliably assessed in the first trimester rather than waiting for a second-trimester blood test or amniocentesis.
Most couples say they are both profoundly grateful for the information and hugely burdened by the choices it forces them to make. The availability of tests earlier in pregnancy means that if they opt for an abortion it can be safer and less public.
But first they must decide: What defect, if any, is reason enough to end a pregnancy that was very much wanted? Shortened limbs that could be partly treated with growth hormones? What about a life expectancy of only a few months? What about 30 years? Or a 20 percent chance of mental retardation?
Decision time
Striving to be neutral, doctors and genetic counselors flood patients with scientific data, leaving them alone for the hard conversations about the ethics of abortion and how having a child with a particular disease or disability would affect them and their families. There are few traditions to turn to and rarely anyone around who has confronted a similar dilemma.
Against the backdrop of a bitter national divide on abortion, couples are devising their own very private scales for weighing whether to continue their pregnancies. Often, political or religious beliefs end up being put aside, trumped by personal feelings. And even many of those who have no doubts about their decision to terminate say the grief is lasting.
"It was never even anything I had considered until I had the bad results," said Hoffman, who ended her pregnancy last year after a followup test confirmed that her child, if it survived, would have Down syndrome. "It was the hardest decision I ever had to make."
She and her husband, Drew, of Marblehead, Massachusetts, decided that the quality of the child's life -- and that of the rest of their family -- would be too severely compromised. "I don't look at it as though I had an abortion, even though that is technically what it is," she added. "There's a difference. I wanted this baby."
Whatever they choose, couples find themselves exposed to judgments from all sides. Several of those interviewed asked that personal details be withheld because they had let friends and family believe that their abortion was a miscarriage. Others say they have been surprised that even conservative parents, who never faced such decisions themselves, have counseled them to abort rather than face too hard a life.
Activists for the rights of the disabled say that a kind of grass-roots eugenics is evolving that will ultimately lead to greater intolerance of disabilities and less money for cures or treatments. And even some doctors who perform abortions are uncomfortable as some patients choose to quietly abort fetuses with relatively minor defects.
No one tracks the number of abortions performed for medical reasons, but obstetricians say several factors are most likely contributing to a growth in their frequency, including broader availability of new screening technologies and more pregnancies among women over 35, who are at greater risk of carrying a fetus with chromosomal abnormalities.
About a dozen tests for genetic mutations that could cause diseases or disabilities in a child are now regularly offered to pregnant women and their partners, depending on their ethnicity and conditions that run in their
families.
More than 450 conditions, including deafness, dwarfism and skin disease, can be diagnosed by testing fetal cells, with more than 100 tests added in the last year alone. African-Americans are widely screened for sickle-cell anemia, and a panel that now includes nine tests for diseases common to Ashkenazi Jews has virtually eliminated the birth of children in the US with Tay-Sachs, a fatal early childhood genetic disorder.
Next month, the Baylor College of Medicine plans to introduce a pilot program with perhaps the largest panel of prenatal tests ever offered. For US$2,000, a pregnant woman will be able to have her fetus tested for some 50 conditions that cause mental retardation.
Quest Diagnostics, a leading provider of medical tests, said prenatal and genetic mutation tests were one of the fastest-growing parts of its business.
"People are going to the doctor and saying, `I don't want to have a handicapped child, what can you do for me?"' said Charles Strom, medical director of Quest's genetic testing center.
The new screening tests provide reassuring news for the vast majority of pregnant women. But Amy D, a preschool teacher in Livingston, New Jersey, who terminated a pregnancy after finding out the child would have cystic fibrosis, remembers falling to her knees in the schoolyard when her genetic counselor called her with the test results.
She and her husband did not know what cystic fibrosis was and had no known family history of the disease, which causes progressive lung failure and carries an average life expectancy of 35 years. But in the fall of 2001, the American College of Obstetricians and Gynecologists recommended that a blood test for the gene mutations that cause the disease be offered in all pregnancies when either the man or woman is Caucasian.
Amy D screened positive as a carrier in August 2002, shortly after she found out she was pregnant with her first child. When her husband also turned out to be a carrier, there was a one-in-four chance that their fetus would have the disease. An amniocentesis showed that it would.
Having watched her husband shrink from scenes of suffering, whether in movies or during his own father's illness, she said she knew her marriage would not survive having a severely ill child. "My life would have been caring for my child, which would have been fine if she would be OK," said Amy D, who asked that her last name be withheld for fear that anti-abortion activists would harass her. "But she wasn't going to be OK."
After months of depression, she said she is thrilled to be adopting an infant boy from Asia. Still, when she watches the 20-something woman with cystic fibrosis on MTV's Real World dating and getting body piercings, Amy D says she cannot help wondering if her daughter, who would have been named Sydney Frances, would have been like that -- at least for a while.
With the number of American couples being tested to determine if they carry cystic fibrosis soaring from a few thousand in 2000 to several hundred thousand last year, more people are tackling similar decisions. Sometimes, the gene tests can even distinguish between a mutation that causes a mild form of cystic fibrosis and one that is more severe.
Termination
When Dr. Janel Crawford, a gynecologist in El Dorado Hills, California, learned that her second child, Hannah, would probably have a moderate case of the disease, she and her husband decided they could not terminate the pregnancy. "All the information starts to make things so complex," said Crawford, who said she had her first big scare when 10-month-old Hannah recently had a cold. "I almost wanted to go to the other extreme and stick my head in the sand like an ostrich and not know."
Kaiser Permanente, a large managed health care organization, said that when both members of a couple among its northern California patients tested positive, 80 percent opted for the follow-up test of their fetus. Of those whose fetus was affected, 95 percent terminated the pregnancy.
"It's a crummy disease, the treatments are far from what we would like, and we have a reliable test," said Dr. David Witt, director of Kaiser's northern California prenatal screening program. "Based on the response, people are grateful they had an opportunity to take advantage of it."
The wider range and earlier timing of prenatal tests are raising concern among some bioethicists and advocates for disability rights who argue that the medical establishment is sending a message to patients that the goal is to guard against the birth of children with disabilities.
"By putting them out there as something everyone must do, the profession communicates that these are conditions that everyone must avoid," said Adrienne Asch, a bioethicist at Wellesley College. "And the earlier you can get it done the more you can get away with because you never have to tell anybody."
Some doctors, too, say they are troubled by what sometimes seems like a slippery slope from prenatal science to eugenics. The problem, though, is where to draw the line.
Dr. Jonathan Lanzkowsky, an obstetrician affiliated with Mount Sinai Hospital in Manhattan, described one woman who had been born with an extra finger, which was surgically removed when she was a child. Her children have a 50-50 chance of inheriting the condition, but she is determined not to let that happen. Detecting the extra digit through early ultrasounds, she has terminated two pregnancies so far, despite doctors' efforts to persuade her to do otherwise, Lanzkowsky said.
Other doctors said that they had seen couples terminate pregnancies for poor vision, whose effect they had witnessed on a family member, or a cleft palate, which they worried would affect the quality of their child's life.
In an extreme case, Dr. Mark Engelbert, an obstetrician/gynecologist on the Upper East Side of Manhattan, said he had performed an abortion for a woman who had three girls and wanted a boy.
"She was much more comfortable with it than I was," Engelbert said. "I told her if it was a new patient I wouldn't have done it. But my feeling as a physician was that I've accepted the responsibility of being her health care provider. She's not doing anything illegal, and it's not for me to decide."
Perhaps the hardest cases for both doctors and patients come when technology provides enough information to raise concerns about the health of a fetus but not enough to make a conclusive diagnosis. When Tom Horan and his wife learned in April that their fetus' legs were bowed and shortened, they were told that the condition could be healed through braces, growth hormones and surgical procedures in childhood.
But before they decided what to do, a closer examination by a specialist with a 3-D ultrasound machine revealed other deformities: The left arm was missing below the elbow, and the right hand was only partially developed. Moreover, sometimes such features are a sign of a neurological impairment, the doctors told them, but in this case it was impossible to tell.
"Our main concern was the quality of life that the child would have growing up with such extensive limb deformities, even in the absence of cognitive problems," Horan said. He and his wife, who have three other children, were reared Roman Catholic and had never considered terminating a pregnancy. Yet even his father, Horan said, who had long been opposed to abortion, supported their decision to end the pregnancy.

The arithmetic is straightforward and uncomfortable. By the end of 2025, Taiwan had committed itself to a 50-30-20 electricity mix — half natural gas, 30 per cent coal, 20 per cent renewables. The Ministry of Economic Affairs’s (MOEA) own monthly energy reports tell a different story. Natural gas reached 47.8 per cent of generation last year. Coal stood at 35.4 per cent, comfortably above its target ceiling. Renewables came in at 13.1 per cent, well short of the 20 per cent Taipei had pledged a decade earlier. Installed renewable capacity reached roughly half of the 12 gigawatts (GW) the government

There are shadowy cabals plotting to sell out Taiwan to be annexed by China, by invasion if necessary. Fortunately, they are buffoons. In 2019, former Bamboo Union gangster and founder of the China Unification Promotion Party (CUPP), Chang An-le (張安樂, colorfully known as “White Wolf”), led a protest at the Legislative Yuan against comments made by then-premier Su Tseng-chang (蘇貞昌) that in the event of an attack by China, he would never surrender, but would protect the nation by fighting to the end, even if he only had a broom. Chang had party members bring a wooden casket that they

It seems every few days one bumps into one of those “real man” comments in which Taiwan is urged to “face reality” or similar, and “make a deal,” with the speaker implying that soon it will be too late. “Deal” advocates always present themselves as having a superior grip on reality, and the manly ability to make the “hard choice.” Their testosterone-laden language often echoes that of Taiwan sellout advocates. Note that such commentary always specifies a process (“make a deal, work with, make progress”), never the end state of what occupation by a violent authoritarian colonialist state will entail. In

Taiwan’s drone exports are taking off, fuelled by the war in Ukraine, as Taiwanese companies seek a stake in the fast-growing global market for unmanned aerial vehicles (UAV). Low-cost drones used for reconnaissance and strikes are in high demand as governments around the world boost defense spending in the face of intensifying conflicts. A relative new player in the increasingly competitive industry, Taiwan’s pitch is to be an “Asian hub” for the production of UAVs and components free of Chinese materials, or “non-red.” That means its UAVs can be up to three times more expensive than their Chinese competitors, like the world’s biggest