The siblings of children with attention deficit hyperactivity disorder (ADHD) are three to four times more likely to be diagnosed with the disorder than children in general, a child psychiatry research team at National Taiwan University Hospital said.
The team, led by the director of the hospital’s psychiatry department, Susan Gau (高淑芬), has spent years building a nationwide ADHD family database by collecting data on patients’ longitudinal follow-ups and clinical, neuropsychological, pharmacotherapeutic, brain imaging and genetic study results.
Gau said the data they have collected indicate that 25 to 30 percent of the siblings of children with ADHD also have the disorder — a figure that is three to four times higher than the estimated prevalence of ADHD in general in Taiwan at 7 percent.
Typical symptoms of children with ADHD include inattention, hyperactivity, impulsivity, difficulty controlling their emotions and problems organizing or completing a task, which could have a negative impact on their performance in school and social interaction.
“While some children may be diagnosed to have the disorder like their brother or sister, there are also those who are ‘in-betweens,’ meaning they have not been diagnosed with the condition, but have been identified as ADHD cognitive endophenotypes,” Gau said.
While ADHD is hereditary, it is a clinically and genetically heterogeneous disorder, the team said, meaning the disorder can be caused, independently, by a variety of genetic defects.
Since the symptoms and signs of the disease — phenotype (observable traits) of the acting genes — can be the result of multiple genetic and non-genetic factors acting in concert, psychiatrists are using endophenotype, which can be seen as a biological marker more proximal to the biological etiology of a disease than its signs and symptoms, “to target the possible pathophysiological deficits that combine to create the overall condition of ADHD,” the team said.
Neurocognitive deficits such as those in sustained attention, cognitive impulsivity, reaction time, time perception, visual memory and various executive functions (eg, working memory, cognitive flexibility, planning and problem solving) are proposed by the team to be the endophenotypes of ADHD as they are shared by both children diagnosed with ADHD and their clinically unaffected siblings.
Gau said she did not want to put emphasis on the number of the unaffected siblings that are found with the said neurocognitive deficits, citing problems of labeling and unnecessary fear.
However, when asked about the problem of “overdiagnosis” of ADHD as some experts abroad have feared, Gau said that while the allegations might stand in some countries where family physicians and pediatricians are making ADHD diagnoses, it is not statistically supported in Taiwan, where the disorder is almost always diagnosed by psychiatrists adhering to recognized diagnostic criteria.
“In Taiwan the disorder is actually underreported,” she said. “Only about a third of the affected have sought medical attention.”
Despite a prevalence of about 7 percent, National Health Insurance registration records show only about 2.5 percent of people with ADHD went to see a doctor.
Gau attributed the underdiagnosis partly to Taiwanese’s aversion to taking drugs, especially for children, and the social stigma associated with psychiatric disorders
Nevertheless, ADHD and autism spectrum disorder (ASD), another disorder that Gau and her team have been studying, are both seeing growth in the number of cases in recent years, a phenomenon she said might be due to the relaxation of diagnostic criteria and the general public’s better understanding of the disorders.
“Environmental factors may have also played a role,” she said, and referred to a recent documentary, Toxic Bees — Nature’s Mayday (蜂狂), produced by Taiwan Public Television Service.
The documentary dealt with the issue of bee colony collapse disorder, which some scientists and public health experts have associated with the use of pesticides.
Gau was featured in the film, explaining the difference in brain activity of children with ADHD and those without.
The film referred to a recent study suggesting children exposed to organophosphates, a kind of pesticide, could be at a higher risk of having ADHD.
The author of the study, Marc Weisskopf, of the Harvard School of Public Health, published another report last year suggesting that prenatal exposure to high levels of certain types of air pollutants is associated with a baby’s increased risk of autism.
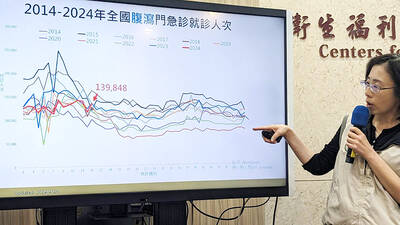
FLU SEASON: Twenty-six severe cases were reported from Tuesday last week to Monday, including a seven-year-old girl diagnosed with influenza-associated encephalopathy Nearly 140,000 people sought medical assistance for diarrhea last week, the Centers for Disease Control (CDC) said on Tuesday. From April 7 to Saturday last week, 139,848 people sought medical help for diarrhea-related illness, a 15.7 percent increase from last week’s 120,868 reports, CDC Epidemic Intelligence Center Deputy Director Lee Chia-lin (李佳琳) said. The number of people who reported diarrhea-related illness last week was the fourth highest in the same time period over the past decade, Lee said. Over the past four weeks, 203 mass illness cases had been reported, nearly four times higher than the 54 cases documented in the same period

A group of Taiwanese-American and Tibetan-American students at Harvard University on Saturday disrupted Chinese Ambassador to the US Xie Feng’s (謝鋒) speech at the school, accusing him of being responsible for numerous human rights violations. Four students — two Taiwanese Americans and two from Tibet — held up banners inside a conference hall where Xie was delivering a speech at the opening ceremony of the Harvard Kennedy School China Conference 2024. In a video clip provided by the Coalition of Students Resisting the CCP (Chinese Communist Party), Taiwanese-American Cosette Wu (吳亭樺) and Tibetan-American Tsering Yangchen are seen holding banners that together read:
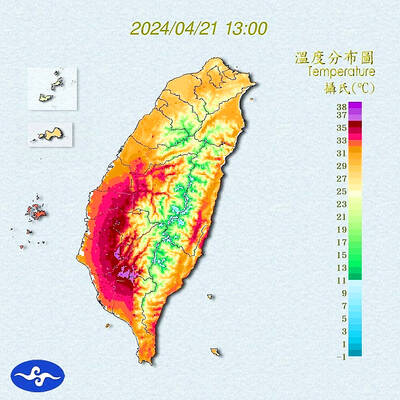
Heat advisories were in effect for nine administrative regions yesterday afternoon as warm southwesterly winds pushed temperatures above 38°C in parts of southern Taiwan, the Central Weather Administration (CWA) said. As of 3:30pm yesterday, Tainan’s Yujing District (玉井) had recorded the day’s highest temperature of 39.7°C, though the measurement will not be included in Taiwan’s official heat records since Yujing is an automatic rather than manually operated weather station, the CWA said. Highs recorded in other areas were 38.7°C in Kaohsiung’s Neimen District (內門), 38.2°C in Chiayi City and 38.1°C in Pingtung’s Sandimen Township (三地門), CWA data showed. The spell of scorching

UNAWARE: Many people sit for long hours every day and eat unhealthy foods, putting them at greater risk of developing one of the ‘three highs,’ an expert said More than 30 percent of adults aged 40 or older who underwent a government-funded health exam were unaware they had at least one of the “three highs” — high blood pressure, high blood lipids or high blood sugar, the Health Promotion Administration (HPA) said yesterday. Among adults aged 40 or older who said they did not have any of the “three highs” before taking the health exam, more than 30 percent were found to have at least one of them, Adult Preventive Health Examination Service data from 2022 showed. People with long-term medical conditions such as hypertension or diabetes usually do not