The Centers for Disease Control (CDC) denied that there has been a drastic increase in the prevalence of HIV drug resistance among people with HIV, which the Taiwan AIDS Society president attributed to the CDC prescribing cheaper medication.
Society president Lin Hsi-hsun (林錫勳) called for the elimination of discrimination against people who are HIV positive at a press conference on Monday, saying that while the US guidelines for the initial combination regimens for antiretroviral therapy (ART) -naive HIV-infected patients, or HIV patients who have never received treatment, take their quality of life into consideration, Taiwan’s authorities see the cost of HIV drugs as the most important factor in their guidelines for treatment.
He referred to a regional study conducted by National Taiwan University Hospital that showed a doubling of the prevalence of HIV drug resistance from 8 percent last year to 16 percent this year.
“There are two possible causes,” Lin said. “One is the CDC’s recommended combination regimens, which were decided upon according to drug price, and this has resulted in our first-line therapy [provided for all ART-naive patients] being the less costly NNRTIs [Non-nucleoside reverse-transcriptase inhibitors], which is also more likely to induce drug resistance.”
“The other possible cause is unsafe sex without using condoms, which can transmit drug resistance virus,” he added.
The CDC later responded to the accusation by saying that a total of four classes of combination regimens have been provided as treatment guidelines.
While the CDC encourages use of the combination regimen that is less expensive, but equally effective, those with serious side-effects or other conditions that prevent the use of certain drugs can be prescribed with combinations that best suit their needs, it said.
The agency also said that the study referred to was regional in character and thereby limited, emphasizing that CDC’s national survey by random sampling recorded drug resistance prevalence of between 6.7 percent and 9.2 percent from 2009 to last year.
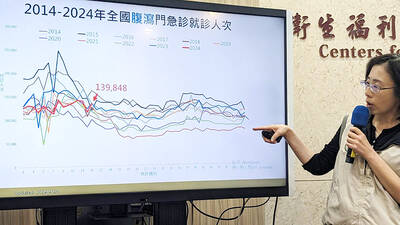
FLU SEASON: Twenty-six severe cases were reported from Tuesday last week to Monday, including a seven-year-old girl diagnosed with influenza-associated encephalopathy Nearly 140,000 people sought medical assistance for diarrhea last week, the Centers for Disease Control (CDC) said on Tuesday. From April 7 to Saturday last week, 139,848 people sought medical help for diarrhea-related illness, a 15.7 percent increase from last week’s 120,868 reports, CDC Epidemic Intelligence Center Deputy Director Lee Chia-lin (李佳琳) said. The number of people who reported diarrhea-related illness last week was the fourth highest in the same time period over the past decade, Lee said. Over the past four weeks, 203 mass illness cases had been reported, nearly four times higher than the 54 cases documented in the same period

A group of Taiwanese-American and Tibetan-American students at Harvard University on Saturday disrupted Chinese Ambassador to the US Xie Feng’s (謝鋒) speech at the school, accusing him of being responsible for numerous human rights violations. Four students — two Taiwanese Americans and two from Tibet — held up banners inside a conference hall where Xie was delivering a speech at the opening ceremony of the Harvard Kennedy School China Conference 2024. In a video clip provided by the Coalition of Students Resisting the CCP (Chinese Communist Party), Taiwanese-American Cosette Wu (吳亭樺) and Tibetan-American Tsering Yangchen are seen holding banners that together read:
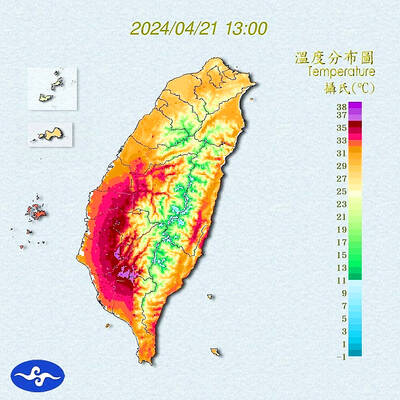
Heat advisories were in effect for nine administrative regions yesterday afternoon as warm southwesterly winds pushed temperatures above 38°C in parts of southern Taiwan, the Central Weather Administration (CWA) said. As of 3:30pm yesterday, Tainan’s Yujing District (玉井) had recorded the day’s highest temperature of 39.7°C, though the measurement will not be included in Taiwan’s official heat records since Yujing is an automatic rather than manually operated weather station, the CWA said. Highs recorded in other areas were 38.7°C in Kaohsiung’s Neimen District (內門), 38.2°C in Chiayi City and 38.1°C in Pingtung’s Sandimen Township (三地門), CWA data showed. The spell of scorching

UNAWARE: Many people sit for long hours every day and eat unhealthy foods, putting them at greater risk of developing one of the ‘three highs,’ an expert said More than 30 percent of adults aged 40 or older who underwent a government-funded health exam were unaware they had at least one of the “three highs” — high blood pressure, high blood lipids or high blood sugar, the Health Promotion Administration (HPA) said yesterday. Among adults aged 40 or older who said they did not have any of the “three highs” before taking the health exam, more than 30 percent were found to have at least one of them, Adult Preventive Health Examination Service data from 2022 showed. People with long-term medical conditions such as hypertension or diabetes usually do not