General Electric Co (GE) and Microsoft Corp plan a joint venture combining electronic healthcare management and software systems that aim to reduce costs from errors and waste of as much as US$500 billion yearly in the US.
The venture, to be run by GE’s Michael Simpson, will have about 700 employees and combine Redmond, Washington-based Microsoft’s systems that use information for billing and patient privacy protocols with GE’s live hospital and patient data system, the companies said in a statement yesterday.
“The global healthcare industry really understands it needs to go after cost, quality and access,” Jan De Witte, who took over GE Healthcare’s information technology division in April, said in an interview. “[In the US] policies are pushing it that direction, and the same is going on in virtually every country in the world.”
The yet-to-be named venture, to be formed in the first half of next year, combines health information exchange and clinical products from GE, the world’s biggest maker of medical imaging and related information systems, and Microsoft’s health management software. Executives said they are seeking regulatory approval in the first half of next year.
GE Healthcare has estimated US$500 billion of the US$2.2 trillion spent on healthcare each year in the US is pegged on duplicate systems and bad coordination, based on US Centers for Medicare and Medicaid Services figures. A Thompson Reuters study in June said US$3.6 trillion could be saved by improvements over a decade.
The companies yesterday cited 1.7 million infections resulting in US$35 billion in excess cost and the loss of 100,000 lives as one area to target with their new products. Chronic disease management and billing system coordination are other potential uses.
The data needed to solve such problems would be developed in an open way, allowing any company to submit an application, and distributed through the venture, Peter Neupert, who runs the health strategy division at Microsoft, said in an interview. The companies didn’t provide a new market size for such tools in part, because it doesn’t exist just yet, he said.
“If you look at the payment models, or bundled payments, or risk-based payment — there’s no software category for that. But those people need tools in order to be able to manage and coordinate care across patients as a group,” Neupert said. “And those are the kind of tools that we can enable and we can build.”

Stephen Garrett, a 27-year-old graduate student, always thought he would study in China, but first the country’s restrictive COVID-19 policies made it nearly impossible and now he has other concerns. The cost is one deterrent, but Garrett is more worried about restrictions on academic freedom and the personal risk of being stranded in China. He is not alone. Only about 700 American students are studying at Chinese universities, down from a peak of nearly 25,000 a decade ago, while there are nearly 300,000 Chinese students at US schools. Some young Americans are discouraged from investing their time in China by what they see
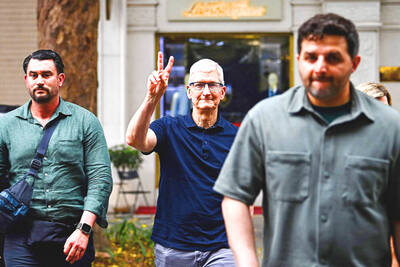
MAJOR DROP: CEO Tim Cook, who is visiting Hanoi, pledged the firm was committed to Vietnam after its smartphone shipments declined 9.6% annually in the first quarter Apple Inc yesterday said it would increase spending on suppliers in Vietnam, a key production hub, as CEO Tim Cook arrived in the country for a two-day visit. The iPhone maker announced the news in a statement on its Web site, but gave no details of how much it would spend or where the money would go. Cook is expected to meet programmers, content creators and students during his visit, online newspaper VnExpress reported. The visit comes as US President Joe Biden’s administration seeks to ramp up Vietnam’s role in the global tech supply chain to reduce the US’ dependence on China. Images on

New apartments in Taiwan’s major cities are getting smaller, while old apartments are increasingly occupied by older people, many of whom live alone, government data showed. The phenomenon has to do with sharpening unaffordable property prices and an aging population, property brokers said. Apartments with one bedroom that are two years old or older have gained a noticeable presence in the nation’s six special municipalities as well as Hsinchu county and city in the past five years, Evertrust Rehouse Co (永慶房產集團) found, citing data from the government’s real-price transaction platform. In Taipei, apartments with one bedroom accounted for 19 percent of deals last

US CONSCULTANT: The US Department of Commerce’s Ursula Burns is a rarely seen US government consultant to be put forward to sit on the board, nominated as an independent director Taiwan Semiconductor Manufacturing Co (TSMC, 台積電), the world’s largest contract chipmaker, yesterday nominated 10 candidates for its new board of directors, including Ursula Burns from the US Department of Commerce. It is rare that TSMC has nominated a US government consultant to sit on its board. Burns was nominated as one of seven independent directors. She is vice chair of the department’s Advisory Council on Supply Chain Competitiveness. Burns is to stand for election at TSMC’s annual shareholders’ meeting on June 4 along with the rest of the candidates. TSMC chairman Mark Liu (劉德音) was not on the list after in December last